The examiner's right hand is then curled over the anterior aspect of the elbow to palpate along the course of the artery just medial to the biceps tendon and lateral to the medial epicondyle of the humerus. To examine the brachial artery ( Figure 30.1) in the right arm, the examiner supports the patient's forearm in his left hand, with the subject's upper arm abducted, the elbow slightly flexed, and the forearm externally rotated. The examiner may be able to see the skin rise and fall with each pulsation along the course of an extremity artery, particularly if a bright light is aimed tangentially across the surface of the skin. Frequently, inspection will be an aid to pulse location. The thumb carries a greater likelihood of confusion with the examiner's own pulse and generally has less discriminating sensation than the fingers. In general, it is inadvisable to use the thumb in palpating for peripheral pulses. The student examiner must be alert to the possibility that the pulse he or she feels may be due to digital artery pulsations in his own fingertips this source of confusion can be eliminated by comparing the pulse in question to his own radial pulse or to the patient's cardiac sounds as determined by auscultation over the precordium. 
Palpation should be done using the fingertips and intensity of the pulse graded on a scale of 0 to 4 +:0 indicating no palpable pulse 1 + indicating a faint, but detectable pulse 2 + suggesting a slightly more diminished pulse than normal 3 + is a normal pulse and 4 + indicating a bounding pulse. A cool environment may cause peripheral vasoconstriction and reduce the peripheral pulse. The patient should be examined in a warm room with arrangements made so that the patient's pulses can easily be examined from both sides of the bed. It is unreliable to attempt to estimate blood pressure via arterial palpation without the use of the sphygmomanometer. While examining the pulse, the observer should note its intensity, rate, rhythm, and if any blood vessel tenderness, tortuosity, or nodularity exists. Thereafter, the sound may no longer be detectable as the volume of blood flow becomes greatly reduced.Ī complete physical examination includes the assessment and recording of arterial pulses in all locations. The sound increases in pitch as the lumen becomes more narrowed to a critical size. In general, bruits are not audible until an artery is approximately 50% occluded. The intensity and duration of the bruit relate to the degree of vessel wall distortion. The sound may originate from a local narrowing or dilation of the vessel itself, or it may be transmitted along the artery from a more proximal lesion in the vascular system. Diminished or absent pulses in the various arteries examined may be indicative of impaired blood flow due to a variety of conditions.īruits are rushing sounds heard over large and medium-sized arteries as a result of vibration in the vessel wall caused by turbulent blood flow. Irregularities in the pulse suggest the presence of premature beats, and a completely irregular pulse implies the presence of atrial fibrillation. Slowing of the pulse rate (bradycardia) may be seen in heart block, hypothyroidism, or with the use of certain drugs (e.g., propranolol). 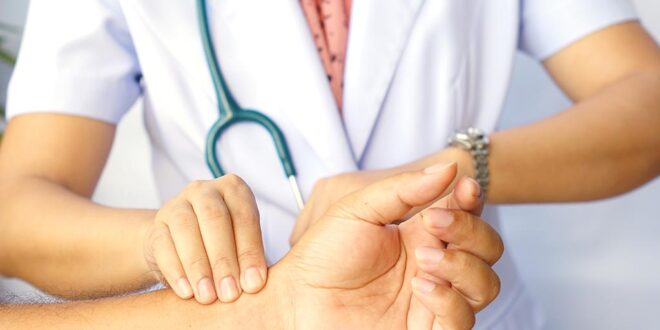
Increases in pulse rate (tachycardia) may suggest hyperthyroidism, anxiety, infection, anemia, or arteriovenous fistula. Assessment of the peripheral vascular system is done to determine the characteristics of the pulse, to ascertain the presence of an arterial bruit(s), and to detect the occurrence of venous inflammation with possible secondary thrombosis of that vein. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
